Patient
A 57 year old female presented with a six month history of cough and shortness of breath. She had been previously treated by her GP with antibiotics and steroids for a suspected respiratory tract infection. An X-ray showed consolidation on the left lower lobe. CT guided biopsy showed a mucinous adenocarcinoma and staphylococcus epidermidis (likely skin contaminant). Decision was made to perform video-assisted thoracoscopic surgery (VATS).
Diagnosis
Following the VATS procedure the lady was diagnosed with a T3N0 adenocarcinoma, and positive parenchymal and peribronchial margins.
Course of treatment
VATS wound was not healing as expected so the patient was referred to Tissue Viability Nurse. Wound was 1x3x2 cm, granulating with low sero-purulent exudate. Wound swab was done to rule out colonisation and showed no growth. Medical team were keen to start combined radiotherapy and chemotherapy, therefore negative pressure wound therapy was considered optimal. SNAP was applied and changed twice weekly.
Plan made with Radiation Oncologist, Medical Oncologist and TVN to proceed with oncology treatment and NPWT in tandem. Radiotherapy was undertaken of 60Gz over thirty fractions to allow skin to recover between fractions. The wound was approximately 7cm from the treated area. Chemotherapy was also commenced, of cisplatin and etoposide50mg/m2 for two cycles of 28 days. Cisplatin causes crosslinking of DNA interfering with replication and synthesis. Etoposide causes breakage errors in DNA synthesis and triggers apoptosis, actively diving cells are more susceptible.
Results
Within one week the wound had decreased to 1×2.7x1cm. After 12 days of SNAP the wound was now superficial and dressing was changed to a disposable NPWT dressing. This was used for a further 10 days before discontinued as the wound had epithelised.
Discussion
VATS wounds usually heal rapidly by primary intention. The patient needed several dressing changes and review by primary care team. Due to non healing wound patients second stage treatment of radiotherapy and chemotherapy was delayed. Therefore the patient had increased healthcare costs and quality of life affected. In addition the patient reported being anxious about wound and relieved when it was healing.
Conclusion
When the decision was taken to start the oncology treatment the aim had been to prevent deterioration and hope for healing. No deterioration of wound occurred despite oncology treatment and the SNAP NPWT system facilitated healing in unfavourable conditions
SNAP system was ideal as it was small, discrete and easily kept out of the field of radiation.
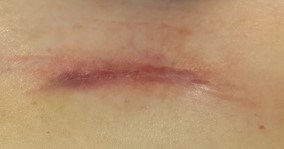
Figure 1 Day 22 post op
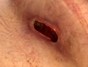
Figure 1 Day 39 post op or Day 7 SNAP
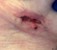
Figure 1 Day 49 post op Day 17 of NPWT
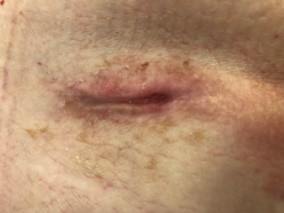
Figure 1 Day 67 post op